When cancer is first diagnosed, it is difficult to predict whether the tumor will recur or metastasize. While most cancers respond well to traditional treatments, if it is not effective, additional chemoradiotherapy may not be advisable.
If traditional treatments do not work, preserved tumor samples can be used to create personalized cancer vaccines. Cancer vaccines train the immune system to recognize and destroy tumor cells in the same way that the immune system reacts to an infection.
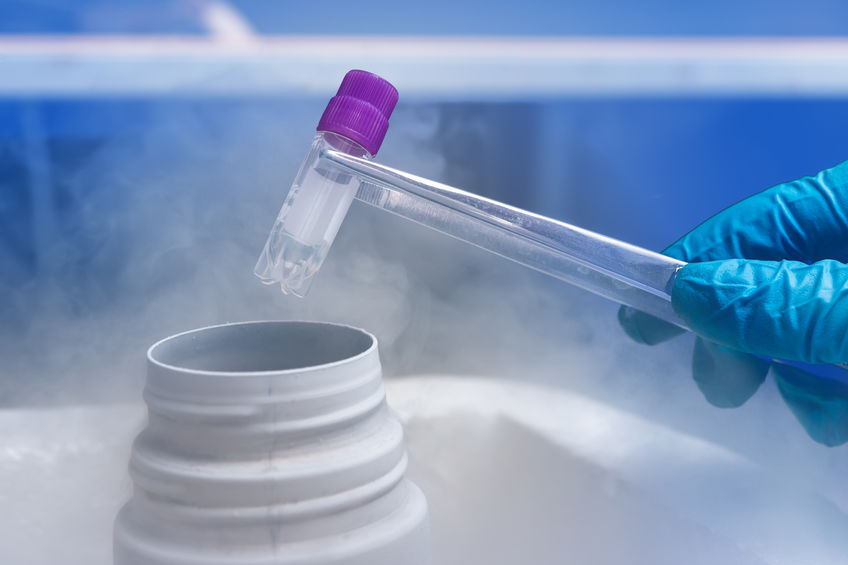
The Tumor Bank stores samples of malignant tumors from patients at extremely low temperatures. By cryopreserving (deep-freezing) tumor samples at extremely low temperatures, we can preserve the “freshness” of cells and the integrity of tumor DNA.
If a patient undergoes surgery, the surgeon should be told in advance if they need to preserve the tumor, so they can try to collect as many undamaged cancer cells as possible. The tumor sample is then placed in sterile, low-temperature-resistant tubes.
Our courier will then deliver the tumor sample to Tel Aviv. Throughout the trip, the tubes are kept in refrigerators at a temperature of -80°C or in liquid nitrogen at -196°C.
Having cryopreserved cancer tissue after the initial treatment course will make it significantly easier to then pursue immunotherapy strategies if they become necessary.
The need for such advanced treatment may be hard to predict during the initial diagnosis process, so the option should always be preemptively considered from the start.
At Biotherapy International, we can preserve cancer tissue and keep it ready to prepare future anti-cancer vaccines, should they become necessary to treat the existing lesion or prevent its recurrence.